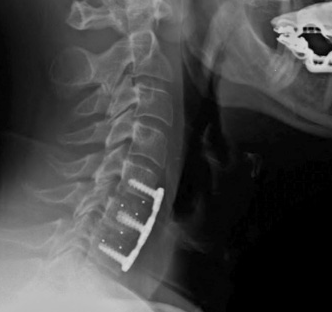
Anterior Cervical Discectomy and Fusion (ACDF)
An ACDF is performed for several reasons, disc herniation or degenerative disc disease is among the most frequent diagnosis. When one or more discs become herniated, they push into the spinal canal and begin compressing the spinal cord (spinal stenosis). A herniated disc can also push to the side and begin compressing the nerve root where it passes through an opening between the vertebrae (foraminal stenosis). Typical symptoms include neck pain that may extend into one or both arms and this is often accompanied by numbness and tingling in the arms and/or hands. Weakness can also ensue depending on the degree and position of the herniation.
Why Neuromonitoring…
During removal of the disc, the surgeon is working very close to the spinal cord and the nerve roots exiting the spine. While the surgeon is removing the disc material, the neurophysiologist uses a multimodal approach to monitor the sensory and motor systems by recording the somatosensory evoked potentials (SSEPs), the transcranial motor evoked potentials (tcMEPs) and the electromyography (EMGs) of myotomes for the appropriate spinal cord levels. Monitoring the SSEPs and tcMEPs provides ongoing check of whether the sensory and motor pathways of the spinal cord are functioning properly and continuous monitoring of the EMG ensures immediate feedback to the surgeon if a nerve root is disturbed.
Once the disc is removed, monitoring continues during placement of the implant. Improper placement could result in compression of the cord or nerve roots.